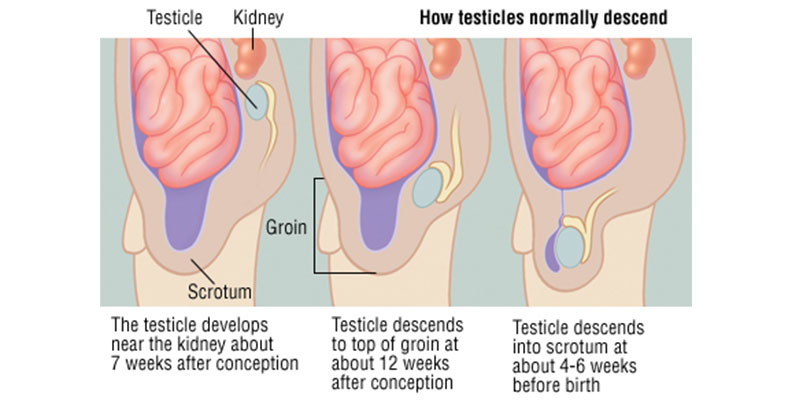
Undescended Testes
An undescended testicle (cryptorchidism) is a testicle that hasn't moved into its proper position in the bag of skin hanging below the penis (scrotum) before birth. Usually just one testicle is affected, but about 10 percent of the time both testicles are undescended.An undescended testicle is uncommon in general, but common among baby boys born prematurely.
The vast majority of the time, the undescended testicle moves into the proper position on its own, within the first few months of life. If your son has an undescended testicle that doesn't correct itself, surgery can relocate the testicle into the scrotum.
SymptomsNot seeing or feeling a testicle where you would expect it to be in the scrotum is the main sign of an undescended testicle.
Testicles form in the abdomen during fetal development. During the last couple of months of normal fetal development, the testicles gradually descend from the abdomen through a tube-like passageway in the groin (inguinal canal) into the scrotum. With an undescended testicle, that process stops or is delayed.
TreatmentIt can be done by Laparoscopic Orchiopexy & Open Orchiopexy Surgery.
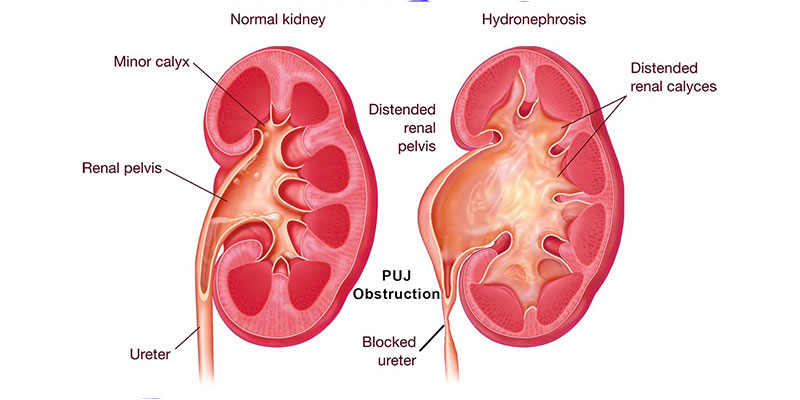
Puj Obstruction
Some children are born with a condition called pelviureteric junction (PUJ) obstruction, which blocks the flow of urine from their kidneys to the bladder. Serious blockage can lead to a deterioration of the function in that kidney , so we asked consultant paediatric urologist Miss Marie-Klaire Farrugia how PUJ obstruction is diagnosed, and when surgery is considered as a treatment option.
Pelviureteric junction (PUJ) obstruction is most commonly due to a narrowing in the part of the ureter which drains urine from the kidney, causing a build-up of urine which then increases the pressure within the kidney - with the potential to cause damage.
PUJ obstruction is most often a congenital condition, occurring in 1 in 1500 births. It tends to affect the left kidney more than the right, but in 10% of cases it affects both kidneys.
What causes PUJ obstruction? PUJ obstruction can be:- intrinsic - the blockage occurs inside, e.g. due to stenosis (a narrowing of the passage)
- extrinsic – the blockage is caused by an external factor putting pressure on the PUJ, such as an extra blood vessel crossing over the ureter.
It can be done by Laparoscopic and Open Pyeloplasty Surgery.
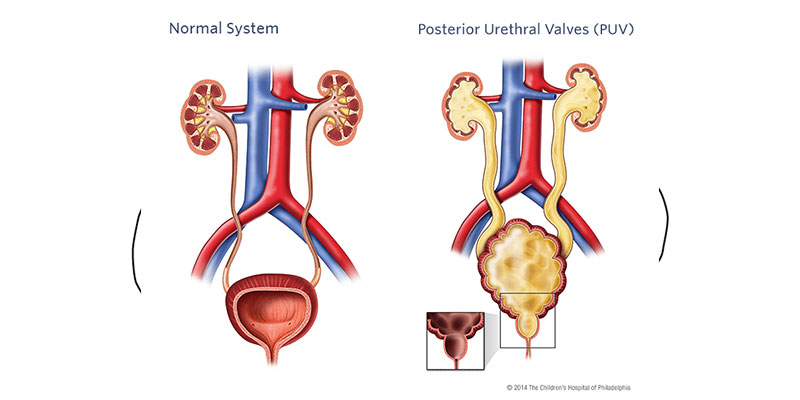
PU Valve Fulguration
Posterior Urethral Valves (PUV) are one of the commonest urolgical problems seen in children and the electrocoagulation, which is the most widely preferred modality to ablate the valves, may not be feasible in small-for-date and low-birth-weight neonates as the suitable size resectoscope/cystoscope may not available. With the availability of Nd: YAG laser at our institute recently, we started performing the laser fulguration instead of electrocoagulation of the valves. We reviewed our experience with the emerging role of the Nd: YAG laser in the fulguration of PUV, comparing the results with a historical control group who underwent the classical electrocoagulation of the PUV. The boys (n=50) diagnosed to have PUV by VCUG were confirmed by Wolf 8.5 size cystoscope, underwent Nd: YAG laser fulguration of the valves with a bare fiber, as a day-care procedure without postoperative catheterization. Historical controls (n=50) who had undergone classical electrocoagulation using 9.5 size Wolf resectoscope served as the controls. The mean age was 1.3 y and 2.6 y in laser and electrocoagulation group respectively. The mean hospital stay of the electrocoagulation group was 3.8 d. Three patients after electrocoagulation developed hematuria and 4 required refulguration whereas in the laser group 5 required refulguration and none developed hematuria. In conclusion, endoscopic laser fulguration of PUV is technically feasible even in neonates and small children. Laser offers excellent results that are comparable to the time-honored electrocoagulation procedure. This has the additional advantage forfulgurating the PUV in smaller caliber urethra as this can be performed with the smaller available cystoscope that has a side channel, admitting the laser fiber.
TreatmentIt can be done by Endoscopic laser Fulguration Surgery.
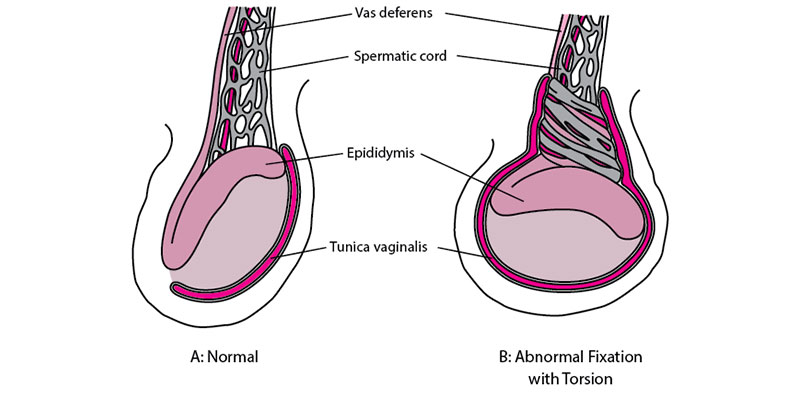
Torsion Testes
Testicular torsion occurs when a testicle rotates, twisting the spermatic cord that brings blood to the scrotum. The reduced blood flow causes sudden and often severe pain and swelling.
Testicular torsion is most common between ages 12 and 18, but it can occur at any age, even before birth.
Testicular torsion usually requires emergency surgery. If treated quickly, the testicle can usually be saved. But when blood flow has been cut off for too long, a testicle might become so badly damaged that it has to be removed.

